Osteoporosis
(Kotsu-soshoh-shoh in
Japanese)
Osteoporosis is a disease
characterized by weak bones due to the reduction of bone density,
a result of decreased bone minerals (calcium and phosphorus) and
protein. The stooped back condition of osteoporosis (we call this
condition a "cat back" in Japan) is the most obvious
symptom. Additionally, fractures occur more easily when lifting
heavy objects, struck on the waist or extremities and following
falls. The cause of the stoop is a compression fracture of the
spine and fore part of the spinal bone as it becomes collapsed.
Patients with osteoporosis will often suffer from hip joint, wrist
and other fractures. These fractures make patients bedridden and
accelerates the deterioration of dementia. This is thought to
be just a senility change, but the cause of osteoporosis is not
only from aging. It is true that elderly people have osteoporosis,
and tha the number of patients with osteoporosis increases proportionate
to aging. One third of the people above the age of 65 have this
disease, and postmenopausal women will develop osteoporosis more
readily than men due to hormonal factors.
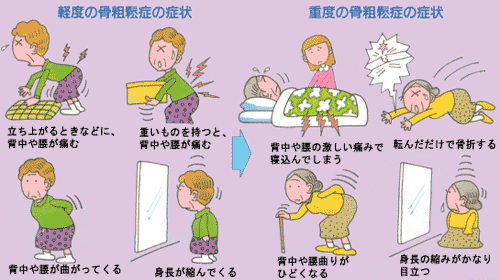
1. Symptoms of Osteoporosis
(1) mild cases
1. Back pain
while standing
2. Back and waist pain while lifting
heavy objects
3. A stoop back
4.
Shrinking height
Spinal bone is a kind of mainstay
of the human body, so a weaker spine results in diminished body
support. This results in the muscles supporting the body instead
of spinal bone, and the muscles will become chronically fatigued.
This is the first stage back pain, so exercise (walking and gymnastics
every day) will be effective to increase muscle power.
According
to the progress of osteoporosis, the following symptoms are recognized;
(2) advanced cases
1. Being
down with back pain and lumbar pain.
2. Hip and
joint fractures from accidental strikes and falls cause many patients
to become bedridden.
3. The stoop can become so
serious that a patient will bend forward severely, causing some
gastrointestinal disorders.
4. Patient's height
shrinks further, and this posture will make a patient be conspicuous,
causing the patient may become timid or depressive.

Sorry, there is only Japanese figure. Left 4 illustration are
mild cases and right 4 illustration are advanced cases. But you
can guess each symptoms by each illustration.
2. The Cause of Osteoporosis
(1) Genetic factor
The period
of menopause, history of delivery, the physique (skinny or slightly-built
old people), family history of osteoporosis and one's race (Asian
people and white people) etc. will influence on the onset of osteoporosis.
(2) Life style
An unbalanced
diet, lack of exercise, excessive taking of alcohol and coffee,
smoking and insufficient sunbath etc. will influence on the early
onset of osteoporosis.
(3) Disease factor
Gastrectomy (resection of stomach), Diabetes Mellitus,
hyperthyroidism, hypercalciuria, medication of steroid, ovarian
dysfunction, primary hyperparathyroidism, renal failure etc will
exacerbate osteoporosis.
3. Diagnosis of Osteoporosis
In a case with back pain or lumbar pain, a case with
fracture on falling down (so-called brittle fracture), the bone
mineral density should be measured.
(1) The
measurement of bone mineral density
There are
some methods such as DXA method (a spinal bone), MD
method (a metacarpus), QTC method and ultrasonographic
method etc, and we examine by MD method at our clinic.
According to the Diagnostic Standard of primary Osteoporosis
(revised in 2000); a case with the data of bone mineral density
of more than 80% of YAM* is regarded as normal; In a case
with the data of 70-80% of YAM, osteoporosis is suspected (it
means reduction of bone minerals), and a case with a history of
fracture and 70-80% of YAM is diagnosed as osteoporosis; a case
with less than 70% of YAM is diagnosed as osteoporosis.
*YAM
: Young Adult Mean data = the mean data of bone mineral density
of 20 - 44 years women
(2) The Marker of Bone
Metabolism
BAP (blood: bone formation),
NTX (blood and urine: resorption of the bone), DPD &
CTX (urine: resorption of the bone) are available, and these
markers can estimate the possibility of fracture and they are
useful for selection of medicine.
�S. The Prevention of Osteoporosis
(1) Walking
Walking for 30 -
60 minutes every day brings good preventive effect.
(2)
Sunbath
Sunbathing helps human metabolism to
assimilate Vitamin D and it builds up bones.
Please
be cautious not to get strong sun rays especially ultraviolet
rays.
(3) Gymnastics & exercise
Training
of back muscles and abdominal muscles prevents chronic tiredness
of bones and resorption of the bones.
(4) Improvement
of eating habits
The content of food is very
important as the following explanation of dietetic therapy.
(5) Bathing and other reluxation
Bathing
(especially Japanese style) reduces muscle contraction and pains,
and makes us feel relaxed.
5. Therapy of Osteoporosis
There are 2 therapeutic points. One is to reduce and
remove lumbar (back) pains, and another is to prevent fracture.
There are physical therapy, dietetic therapy and medicines, and
there are various kinds of medicine for every indication.
(1) Physical Therapy
A. Exercise
Cure
Proper exercise is necessary for the prevention
of osteoporosis and increase of bone minerals. In the acute stage,
exercise should be restricted, but in the chronic stage the aerobics
and exercise for low back management are easy and effective.
B. Physiotherapy
Thermotherapy
(the Embrace III and the microwave therapy at our clinic etc),
phototherapy, electrotherapy and massage are effctive to reduce
pains themselves and analgesic medicine dosage and so side effects
of them.
C. Hip Protector
Prevention
of the femoral neck fracture.
(2) Dietetic Therapy
It is important to avoid undernourishment and an unbalanced
diet. You shoould take not only adequate calcium but potassium,
magnesium and vitamins especially Vitamin D, C and K, and enough
proteins. Also it is important not to increase your body weight
( heavy weight can be a overload to bone and muscles.).
In
the standard for Japanese people recommended by Japanese Ministry
of Health, Labour and Welfare, we should take 600mg of calcium
a day, and aged people and postmenopaused women should take more
than 800mg of calcium a day. Taking dairy products (200 - 400
ml of milk every day), soybean products such as tofu, vegetables
with rich Carotin, fish and shellfish are recommended. On the
other hand, overtaking of salt, caffein, alcohol, vitamin A, precooked
food (fast food) with much phosphorus that disturbs absorption
of calcium, and smoking will aggravate osteoporosis, so you should
be cautious for dietary habits.
(3) Medicine
By Japanese Therapeutic Guideline for Osteoporosis
revised in 2002;
A. Estrogen complex
Estrogen complex is often used for postmenopausal
women with high risk of fracture, because estrogen inhibits the
resorption of the bone (elution of calcium from bone) both directly
and indirectly. Estrogen complex is a hormonal agent, so it has
a side effect to increase the possibility of breast cancer.
B. Bisphosphonate
This has become
a main medicine recently. This medicine has both strong inhibitor
action for resorption of the bone and further calcification of
bone, so good therapeutic effect can be expected for especially
postmenopausal women (etidronate). As the side effect,
there are gastrointestinal disturbance such as nausea and ulcer
formation etc. Alendronate, a kind of biphosphonate, is
useful for men with osteoporosis and especially steroid osteoporosis
by both reliable action to increase bone minerals and to prevent
fracture. And, risedronate has an action to increase bone
mineral density for every aged person with no relation to passing
years of postmenopause. So this medicine may be used for the fixed
case of osteoporosis diagnosed by the association of bone metabolism.
C. Calcium complex
In a definite
case of calcium deficiency disease or condition such as gastic
resection, intestinal resection, anorexia nervosa, excessive poor
appetite and lactose intolerance, calcium complex should be used
with other medicine.
D. Calcitonin complex
Calcitonin acts to the osteoclasts directly and controls
resorption of the bone, then acts as the central analgesics. It
is effctive to reduce back pain and lumbar pain, but it is the
parenteral injection of every week, so an injection itself may
become a kind of torment and a patient sometimes feels nausea
as a side effect, so the patient may abandon this treatment.
E. Steroid for assimilation of protein
This promotes the ossification (bone formation). But
recently this medicine is not so used.
F. Activated
vitamin D3 complex
Vitamin D helps absorption
of phosphorus and calcium in the intestine, and it also controls
synthesis and secretion of PTH (parathormone) in the parathyroid.
This medicine is used for cases of senile osteoporosis of more
than 70 year old and cases of gastric resection and intestinal
resection in which the absorption of calcium may be disturbed.
Overdose of this medicine increses calcium concentration in blood
and it may be a cause of calculus. ED-71 which is highly specific
to bone has been developed recently.
G. Vitamin
K complex
This medicine has weak action to
increase bone minerals, but the preventive action for fracture
has been reported. Various vegetables, meats, eggs and fermented
soybeans (Natto) have rich vitamin K, so vitamin K complex is
uaually used according to the patient's condition and dietary
habits.
H. Ipriflavone
This
medicine is non-hoemonal flavonoid and its action is mild for
both bone formation and resorption of the bone. It can be adapted
to just menopausal women and women with ovarial resection, and
also old aged women.